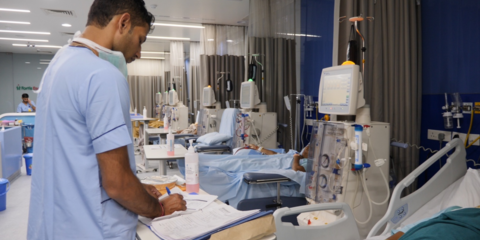
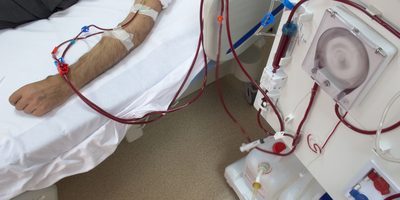
Renal and metabolic
Background
The global burden of kidney disease, both in the form of acute kidney injury and chronic kidney disease, continues to rise as patients are becoming older, sicker and frailer. The high prevalence of chronic conditions such as high blood pressure and diabetes, along with improvements in heart disease survival, are resulting in populations that require more complex medical care and are more susceptible to adverse events that impact upon kidney function. It is estimated that the number of people requiring treatment for end-stage renal disease will more than double between 2010 and 2030.
Around 10% of the world’s population is affected by chronic kidney disease, with socio-economically disadvantaged groups bearing a greater burden, and millions die annually for want of affordable treatment.
At The George Institute, the Renal and Metabolic team conducts research to address these challenges through:
1) Targeting knowledge gaps
We focus on identifying and addressing the knowledge gaps with the biggest impacts on the outcomes of patients with kidney disease. Our teams conduct trials and epidemiological analyses of large datasets to determine the incidence, prevalence and severity of the disease, as well as factors that might influence the burden and improve outcomes for patients. We also develop novel datasets that provide new insights, such as developing research infrastructure in Zimbabwe to enable the first data on the national prevalence and incidence of dialysis.
2) Building global collaborations
Wherever the opportunities and needs lie, we will explore them. We do this through building research collaborations locally, regionally and globally that use existing data, as well as developing new datasets to address key questions in the treatment of kidney disease. Those datasets include administrative data from government collections, existing clinical trials, as well as custom-built epidemiological and clinical trials data drawn from more than 25 countries, in particular the Asia-Pacific region.
Many of the profound challenges in kidney disease will not be met by local initiatives alone. Slowing the progress of diabetic kidney disease is perhaps the most pressing challenge facing global nephrology, and our team has been central to global studies of new treatments that promise to truly transform the treatment of diabetic nephropathy

3) Increasing patient access
Millions of people globally die unnecessarily every year because they cannot access treatment for kidney failures such as dialysis or a kidney transplant. Socio-economically disadvantaged groups in lower-income countries without a social safety net are particularly vulnerable due to treatment costs and distance challenges, which can inflict catastrophic health costs upon patients and their families.
To address these issues, our researchers examine the extent of under-treatment for end-stage kidney disease and develop innovative interventions to increase patient access to proven treatments. Research is focused on determining ways to develop treatments that are affordable, that governments are willing and able to pay for, and then having them delivered close to home in a sustainable way.
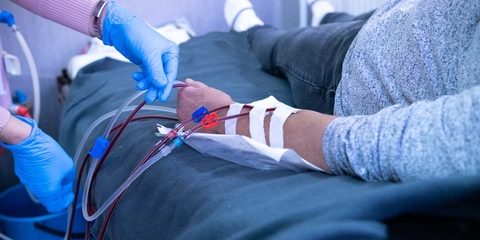
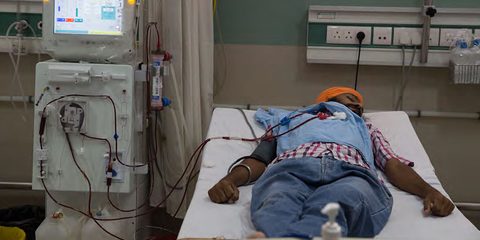
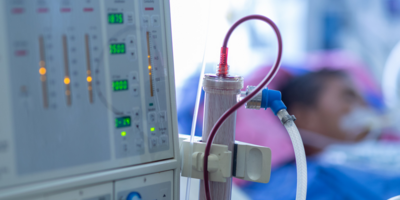
For example, the Affordable Dialysis Project, which involves the design and roll-out of a portable and relatively low-cost dialysis machine, seeks to challenge the existing dialysis business model by delivering cheap, transportable treatment to patients that could otherwise not access the life-saving care. It could save millions of lives each year and transform the way end-stage renal disease is treated around the world.
4) Simplifying treatment
Our research also examines long-established, but poorly studied treatment models that are still widely used but may complicate healthcare or not improve patient outcomes. We aim to simplify healthcare, making it easier to deliver whilst enhancing patient outcomes.
For example, we examined the amount of dialysis that should be used for patients with end-stage kidney disease, as observational data had suggested a benefit from more hours of dialysis every week. Our team conducted a comprehensive trial that found no improvement in patients’ quality of life with more dialysis hours.

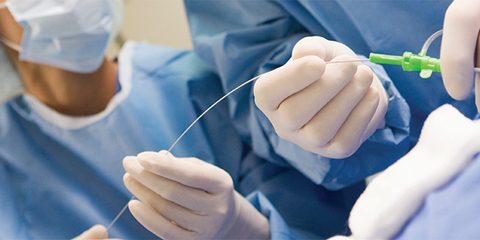
In another trial, our researchers, working with collaborators from the Veterans’ Administration in the US, examined two different treatments widely used to protect patients while they are undergoing angiography. These treatments have been around for almost 20 years and are widely used in the millions of angiographic studies done globally every year. We found that these agents did not make a difference to patient outcomes, with guidelines promptly changing after the study was published to recommend against their use.

5) Improving safety/efficacy of medication
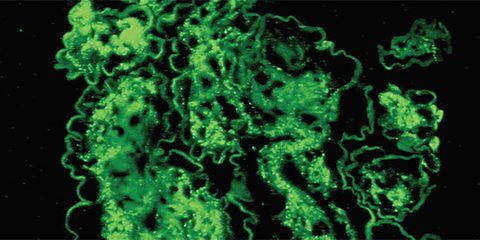
We also examine the harms and risks of legacy kidney disease treatments that have not been rigorously evaluated. For example, we studied whether a corticosteroid treatment, which had been used for over 40 years in treating kidney disease, slowed the progression of the most common immune kidney disease (IgA nephropathy), which has a huge burden in Asia. Most importantly, we also robustly measured the adverse impacts of the treatment, allowing a unique understanding of both the benefits and harms of this treatment. The study findings have played an important role in clinicians re-evaluating the amount of corticosteroid used, and being especially conscious of the potential harms.