
‘Vegemite wouldn't be banned, it would just carry a salt warning'
First published in Australian Doctor
Professor Bruce Neal is one of Australia’s top clinical researchers whose work has exercised a heavy influence over general practice. Here he speaks with Australian Doctor.
"We revile this notion of a nanny state, but we accept this ‘big business’ state that actually does incredible harm,” says Professor Bruce Neal.
“Everyone thinks they’re free-moving individuals making these highly informed choices, but no — they aren’t. They make the choices that big business lets them make.”
Professor Neal is one of Australia’s top public health researchers and like many of his ilk, he sees his role extending beyond the academic, beyond the statistical analysis of population studies, into the political hue and cry.
A few months back, the director of the George Institute’s Food Policy Division was named one of the World’s Most Influential Scientific Minds by the publisher Thomson Reuters, which tallies academic citations. Only six Australian-based researchers have made it to the list.
He is also a researcher whose work has exercised a strong influence over the day-to-day clinical practice of GPs. The shift a decade ago towards focusing on blood pressure reduction outright, regardless of the drug regimens, came largely as a result of the work he has led.
Professor’s Neal says his special talent is designing and analysing big clinical trials. By co- founding the international Blood Pressure Lowering Treatment Trialists’ Collaboration in 1995, he enabled researchers to collect data from some 200,000 subjects on the comparative benefits of ACE inhibitors, or calcium-channel blockers and ARB-based regimens.
The two studies, published in the Lancet in 2000 and 2003, showed that risk of cardiovascular events fell proportionally to the reduction in blood pressure, and chalked up 4000 citations between them.
Professor Neal says: “They have undoubtedly changed the care of literally millions of people because of the influence they’ve had on guidelines.”
The Collaboration’s more recent work has underpinned recommendations for treatment based on absolute risk, not just blood pressure, and has also highlighted diabetes as a major risk.
Off the farm
Currently professor of medicine at the University of Sydney, Professor Neal grew up in East Anglia in the UK. After leaving boarding school, he opted to study veterinary science, because at the time it was “the hardest course to get into”.
“I took a year and went and worked on a bunch of farms in New Zealand, and I realised there was no way I was going to be a vet,” he adds with a laugh. “I wasn’t bothered by the farm work — I just realised that looking after people was going to be way more rewarding than looking after sheep.”
He switched to medicine instead, and after five years of hospital practice, was wondering what speciality he would go for. Then he got a call from a friend who said they needed someone to co-ordinate a global study for a blood-pressure intervention on stroke outcomes.
He protested that he had little expertise for the job.
“And my friend said, ‘I know you’ve never done any research but you produced theatrical plays at uni, didn’t you? If you can organise that, you can run a research project.’
“That was the defining moment for me.”
Taking on the industry
The nature of Professor Neal’s politics can be gauged when he talks about the ‘Big Food’ industry. For a decade now, he has railed against its influence on our lives.
Accusations that public health lobbyists want to confront this commercial force by engineering a ‘nanny state’ are unfair, he says.
It’s “patronising” to blame individuals for bad food choices since the food industry, in its search for profits, exercises so many controls over the options available to them.
The lack of transparency in most food advertising and in basic food labelling has made it almost impossible for them to avoid the choices that so often damage their health.
As senior director of the Food Policy Division at the George Institute, Professor Neal says the “social norm” toward food manufacturing and consumption needs to change.
“The view that I take is that it’s a systems problem. What I want to figure out is how we can turn that around in terms of economics and food supply.”
Big Food is rapidly learning the playbook of Big Tobacco, according to Professor Neal. He accuses industry-funded studies of manipulating the research on the harms of salt on blood pressure and cardiovascular disease.
The findings only appear equivocal because there is “an imperfect evidence base open to manipulation and misinterpretation, and strong commercial interests vested in one side of the case,” he wrote in a scathing commentary in the International Journal of Epidemiology in February this year.
“Together with sugar and fat, salt can transform cheap, low-quality base ingredients into high- value merchandise. Transnational food companies are among the largest businesses in the world and fiercely protect their commercial positions.”
Unfortunately controversial studies get disproportionate publicity even if done poorly, Professor Neal tells Australian Doctor.
“It’s very easy to get yourself published or heard in the general media by highlighting your particular piece of research that doesn’t quite fit in,” he says.
“And because food is a great way to sell copy, the media jump all over it.”
This makes it hard to get a clear public health message across to the public.
Professor Neal’s current focus is to apply the scale and rigour of clinical research to questions of nutrition in industrial food production. For instance, do front-of-package labels change shopping habits of individuals? Do government-decreed limits on salt or sugar content actually make a difference to the manufacturers? Do the ‘serving sizes’ defined by industry mean anything at all in terms of nutritional advice that affects behaviour?
Labelling food
It will be of little surprise to learn he has been at the centre of the food labelling debate in Australia.
While Federal Government was floundering in the face of industry resistance about how to put stars on food packaging to allow customers to distinguish from the good, the bad and the ugly, his team at the George Institute developed FoodSwitch, an app that allowed people to use their smartphones to scan bar-codes and get clear nutritional information on what they were considering putting into their trolleys and whether there were healthier alternatives.
It was a big success, with some 750,000 downloads not just in Australia, but also New Zealand, the UK, China and India.
Professor Neal wants to collect hard evidence that can be used to compel tighter quality regulation, and to name and shame those producers that profit from peddling harmful foods.
In the case of smoking, he says policy change was essential to lead the way, and public sentiment eventually followed — “albeit it took 75 years”.
Food fads
When it comes to the nutritional benefits of what nations eat, public health activists have to ride the wave of consumer fashion — from the Atkins diet to Gwyneth Paltrow and the health wonders of alkaline food.
Professor Neal has spent a career warning us about the dangers of excessive salt intake. But today you can’t open the pages of a newspaper, fitness magazine or woman’s weekly without reading about the dangers of sugar. Professor Neal is accepting.
“Yeah there are mixed messages and the fads are problematic. But I don’t see us as fighting sugar for space. I see the current debate as an opportunity to get food on the agenda generally.”
He also accepts his push to drive down the salt content of packaged foods has always carried with it particularly cultural risks in his adopted country, given the message puts him on a collision course with the one food that has — for reasons that don’t always seem clear — come to symbolise the Australian way.
“Vegemite would not be banned,” he laughs. “I don’t want death threats. But it would be expensive, because it’s taxed and it would carry a clear warning label, ‘TOO MUCH SALT CAN KILL. USE SPARINGLY.’”
On accusations of a geopolitical bias, Professor Neal says “I was never a Marmite fan either.”
Want food advice? Switch on your smartphone
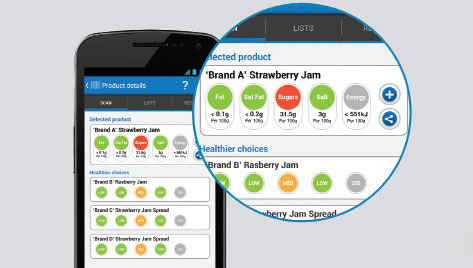
In 2012, Professor Neal launched the Foodswitch smartphone app. It helps people find attractive alternatives to their regular shopping items, and can be tailored to specifically minimise salt, fat or sugar content.
The app has had about 750,000 downloads — not just in Australia, but also New Zealand, the UK, China and India.
But Professor Neal says the vision is much greater than to simply advise a few shoppers as they drift down the aisles at Coles.
“Even with three quarters of a million downloads of an app you’re probably only going to influence the food choices of a few tens of thousands of people. That’s never going to resolve Australia’s health, let alone the world’s.
“But the second part of Foodswitch is we crowd-source a whole load of information about packaged food content,” he says. “Out of the goodness of their hearts, people take photos of products that are missing from the app. We’ve had more than half a million photos sent to us over the last four years and the vision is to go out there and collect information from 50 countries in the next five years.”
Such crowd-sourced data would allow them to massively upscale studies such as their 2011 expose on the salt content of packaged breads. In that study, the researchers themselves had to systematically collect information on Tip Top and WonderWhite and every other such product in the land. They found that three years after national targets for salt content were put into place, the proportion of compliant products had climbed from 29% to about 50%.
They were able to point the finger at those manufacturers whose products didn’t comply, and showed how far behind New Zealand’s 90% compliance rate the Australian industry was.
Australia now has a government-backed alternative in the form of the star ratings. It underwent a painful birth, with complaints from the Australian Food and Grocery Council — Big Food’s industry group — that it would be too expensive to implement, coming up with a figure of $700 million to back their claims.
However, Professor Neal thinks the system launched in 2014 is a good start, though the government shied away from making it mandatory.
“It’s imperfect, but it makes a pretty good assessment in the vast majority of cases,” he says. “I just think we should have it not just on packaged foods but also on restaurant foods.”


